The Death of the 30-Day Rehab (And Where the Smart Money is Going Next)
The trendline is clear.
Welcome to issue #007 of The Patient Pipeline. Each week, I send you an essay to help you become a better healthcare entrepreneur. I’ll give you a digital lead gen audit for free.
I am very passionate about the behavioral health industry.
I have personally been sober for 16 years. I never would have survived without my 30 day treatment program, as the program helped me detox and got me started on my journey.
It makes me nervous to see the trendline of inpatient behavioral health facilities declining. But when you look below the surface, the data tells a fascinating story about where the industry is actually heading. Let us look at the numbers.
First, Let Us Look At The Numbers
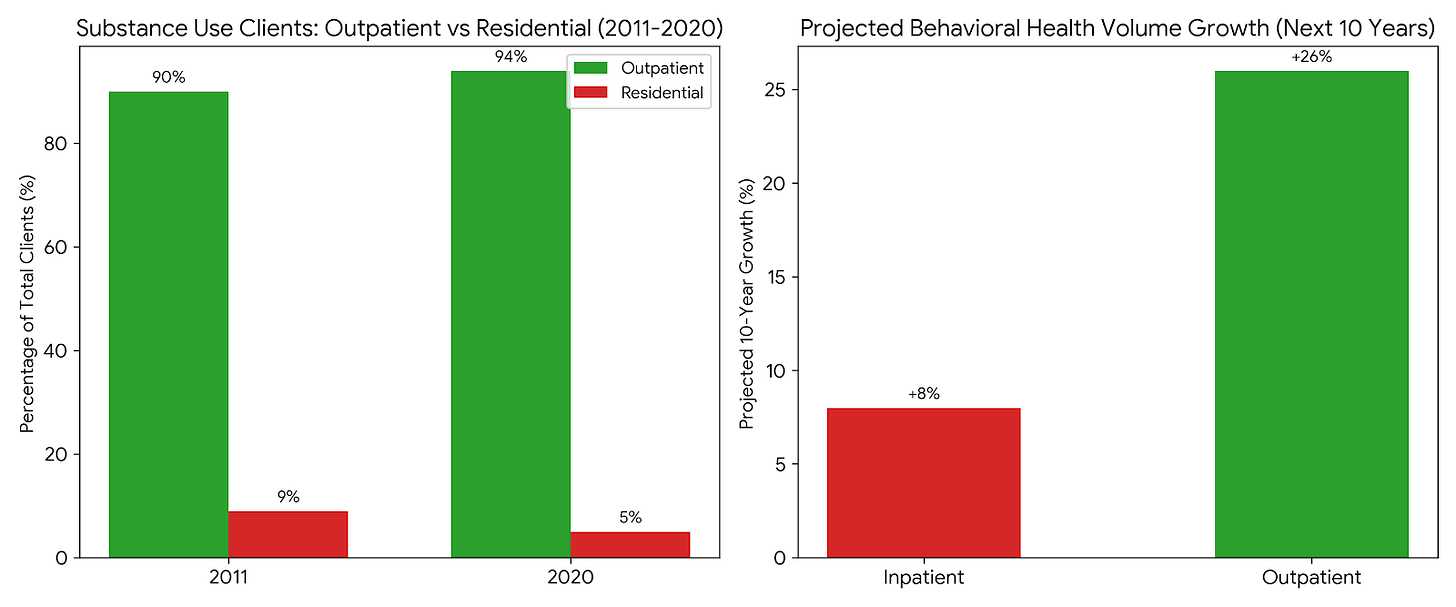
According to the National Survey of Substance Abuse Treatment Services (NSSATS) tracking data from 2011 to 2020, we saw a massive structural shift in where patients were placed:
Residential Decline: In 2011, residential treatment accounted for 9% of all clients in the system. By 2020, that number had nearly halved to just 5%.
Outpatient Growth: Over the exact same period, the proportion of clients treated strictly in outpatient settings increased from 90% to 94%. (Given the millions of Americans in treatment, a 4% total system shift represents hundreds of thousands of patients diverted away from beds).
Inpatient Stagnation: True hospital inpatient care remained entirely flat, hovering between just 1% and 2% of all clients.
When you break down the math, you see an interesting trend.
Overall, there are MORE people attending addiction treatment programs over the last 5 years. But almost all of those people have decided to do outpatient as opposed to inpatient.
So the addiction treatment market has grown, but almost all the growth has gone to outpatient.
Why Inpatient Programs Are Struggling So Bad
It is easy to look at the numbers and conclude that the demand for inpatient treatment is shrinking. That is not what is happening. It is that the economic model for inpatient treatment is facing a lot of structural challenges.
Fundamentally, there are two issues.
The Zoning Squeeze and Regional Hotspots
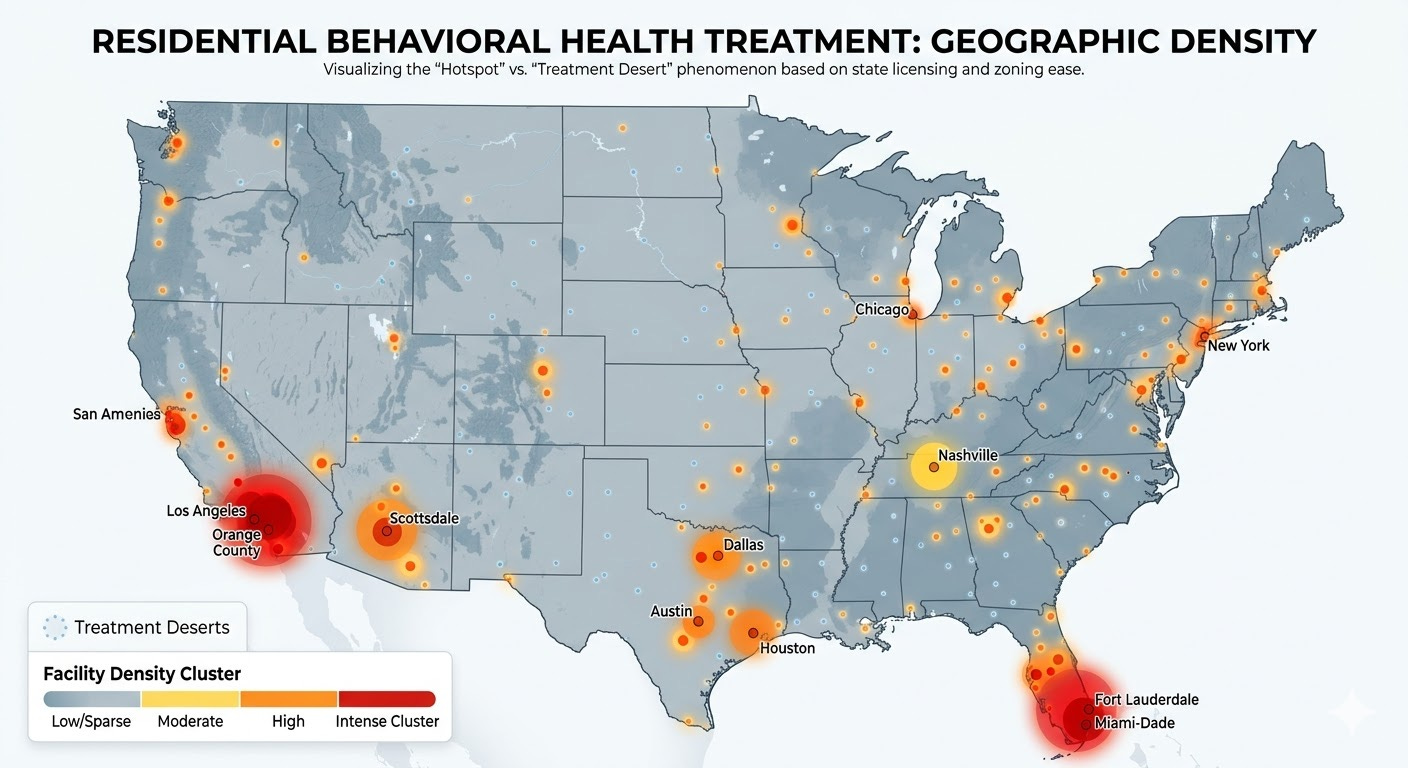
If you look at a map of premium inpatient treatment centers in the United States, you will not see an even distribution based on population need.
The vast majority of facilities are in:
Los Angeles
Orange County
South Florida
Arizona
Texas
Tennessee
This lopsided market is not an accident. It comes down to the path of least resistance in commercial real estate, zoning, and licensure.
The inpatient density problem has created stiff competition in these areas. So instead of an inpatient treatment landscape that is evenly spread, all the facilities are fighting for the same business in the same population centers, and then spending hundreds of thousands of dollars on advertising to try and convince potential clients to fly to those specific locations.
The Payer Problem: Why Insurance is Killing the Model
Even if a facility survives the zoning wars and fills a bed, they immediately face an even bigger hurdle: actually getting paid.
The behavioral health insurance model is fundamentally broken, actively disincentivizing the inpatient care model.
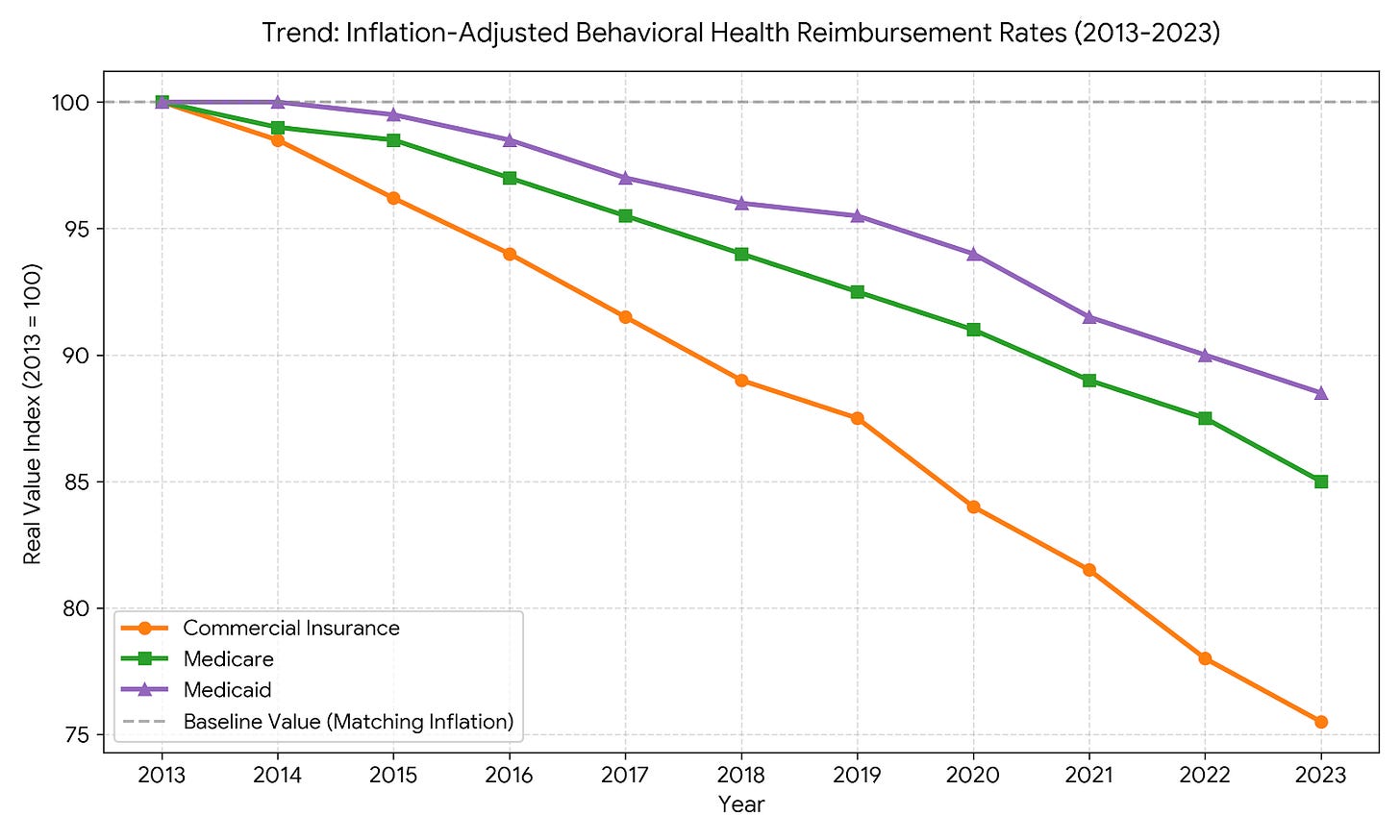
According to the APA official report, reimbursement rates have been rapidly declining.
Here is a breakdown of why the payer system is currently a nightmare for operators:
Weaponized Utilization Management (UM): Insurance companies use aggressive Utilization Management to avoid paying for expensive 30 to 90 day residential stays. They implement incredibly strict medical necessity criteria, often demanding that a patient fail multiple times in a cheaper, outpatient setting before they will approve an inpatient stay.
The Concurrent Review Chokehold: Even if an insurer approves an admission, they rarely approve the whole stay. Clinicians are forced to get on the phone with insurance reviewers every few days to justify why the patient still needs to be there. The moment the insurer decides the patient is no longer in an acute, life threatening crisis, they cut off funding and force a discharge, regardless of whether the clinical team believes the patient is actually ready to go home.
Abysmal and Decreasing Reimbursement Rates: Despite inflation and skyrocketing costs for 24/7 nursing and clinical staff, commercial insurers and Medicaid continuously squeeze behavioral health rates. Studies consistently show that behavioral health is reimbursed at significantly lower rates than standard medical and surgical care. As insurers push for Value Based Care models, they are actively slashing fee for service rates for inpatient beds to force the industry toward cheaper outpatient clinics.
The Illusion of Parity: While the federal Mental Health Parity and Addiction Equity Act legally requires insurers to cover mental health the same way they cover physical health, enforcement is notoriously weak. Insurers skirt the law through administrative burdens, burying facilities in prior authorization delays, retroactive claim denials, and grueling appeals processes until the facility simply gives up or goes out of business.
Why Outpatient Clinics Are Where The Future Is Heading
With inpatient care becoming a logistical and financial nightmare, the smart money and the best operators are moving elsewhere.
The economics are undeniable.
The outpatient treatment model provides a much healthier economic ecosystem for a business to thrive. As far as I can tell, the outpatient model is a much better business opportunity.
Specifically, there are three advantages of outpatient.
First, it is much easier to generate patients from a local level. I have written extensively about local SEO, GBP, and local advertising in my newsletters, and local search still provides the lowest CPA and the best bang for your buck in terms of patient acquisition.
Second, the government and payers are incentivizing behavioral health clinics towards Value Based Care, which rewards keeping patients out of expensive hospital beds. A procedure performed in an outpatient clinic or Ambulatory Surgery Center (ASC) can cost an insurer 30% to 50% less than the exact same procedure done in a hospital.
Third, the outpatient model is an easier system to manage, as it does not require the overhead of living quarters, vans, 24/7 staff, food, and leases.
In Conclusion: Small But Profitable
Over my career as a healthcare entrepreneur, I have seen many inpatient clinics have success and I have seen just as many (if not more) inpatient startups crash and burn. (I have invested in a few myself, but who is counting? lol)
Moving forward, we will continue to see the market reward local outpatient clinics. People who need help would prefer driving to their treatment and going home, rather than committing to a 30 to 90 day stay at an inpatient facility.
The model has limitations, as scaling an outpatient clinic requires you to have multiple locations. The profit margins are healthy, but the limitation is on topline revenue.
Regardless, if you are looking to make money and live a relatively stress free lifestyle, then a well run outpatient clinic is the best opportunity I see.
This is true for all industries, not just behavioral health.
Talk to you next week.
Tim
P.S. - I am combining The Patient Pipeline into my personal Substack. I’ve recently discovered you can run multiple newsletters from one Substack publication. Nothing changes for you, just know that the previous issues will no longer be on patientpipeline.substack.com and will now be found at timstodz.com/healthcare-business.
Scale Your Healthcare Clinic With A Predictable, Automated Patient Acquisition System
Book a call and I’ll provide you with a free digital marketing audit and strategy. No catch. No commitments.
When you partner with our agency, you will get a proven, done-for-you system to generate high-value patients on demand.
You’ll have access to …
custom-built digital marketing campaigns tailored specifically to your practice
exclusive, high-converting patient leads in your local market (we never share leads)
real-time pipeline tracking, so you always know your exact return on investment
monthly strategy reviews with our media buyers to optimize and scale your patient volume
If you’re ready to level up your patient acquisition system, then click the button below and fill out the form.
Let’s grow your practice together.